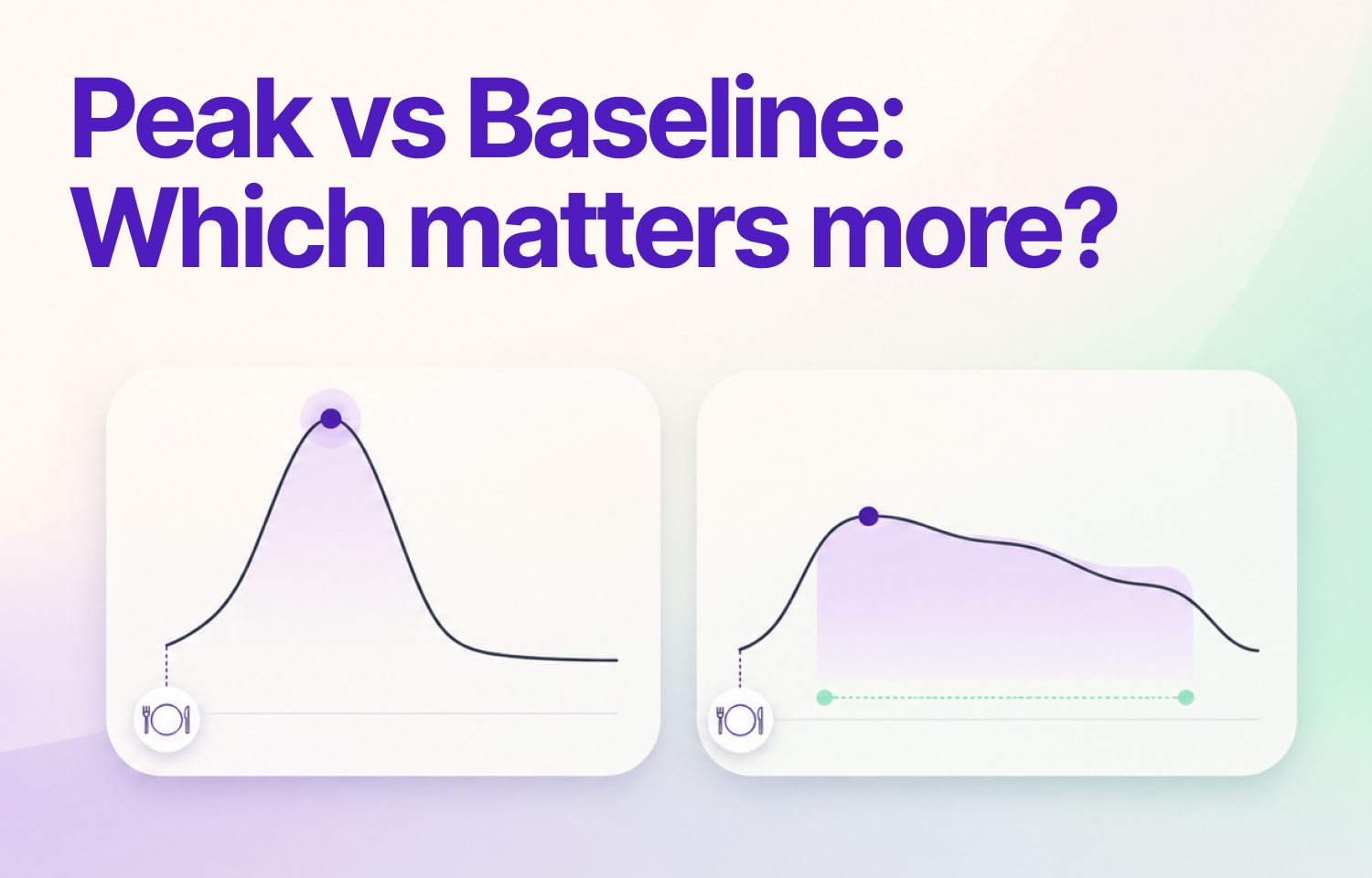
You check your blood sugar before lunch: 142 mg/dL. Two hours later, it's 201 mg/dL. Was it the sandwich? The chips? The timing? Without a continuous glucose monitor, you're left guessing.
But fingerstick testing paired with structured meal tracking can still teach you a lot when managing your diabetes. You won't see the real-time curve that a CGM provides, but you can spot patterns, test hunches, and make smarter food choices over time. Here's how to build a meal-learning system using the tools you already have.
Start With a Testing Rhythm That Actually Teaches You Something
Random fingerstick tests don't reveal much. To understand how a meal affects your blood sugar, you need a before-and-after snapshot.
The American Diabetes Association recommends individualized testing schedules, but a practical starting point is testing before eating and two hours after your first bite. That two-hour window captures the peak glucose response for most meals.
Pick one or two meals per day to track closely. You don't need to test every meal forever. Focus on the meals that feel unpredictable or the ones you eat most often.
If you're trying to figure out a specific food, test it multiple times. A single data point might reflect your stress level, your sleep, or whether you walked after eating. Three or four tests of the same meal give you a clearer picture.
Keep a Meal Log That Goes Beyond "What I Ate"
A list of foods won't teach you much. The details matter.
For each tracked meal, write down:
- What you ate (be specific about preparation: baked vs. fried, white rice vs. brown)
- How much (use measuring cups or your phone's camera for visual reference)
- Carbohydrate count (estimate using a nutrition app, package label, or carb counting guide)
- Blood sugar before and after (include the time of each test)
- Context notes (Did you walk after? Skip breakfast? Feel stressed?)
Context is where the learning happens. You might notice that pasta at lunch spikes you more than pasta at dinner. Or that a 30-gram carb meal paired with a walk barely moves your number, while the same carbs sitting still sends it high. Those patterns can reveal a lot about what really drives your glucose response.
Some people use a notebook. Others prefer a spreadsheet or notes app. The format doesn't matter. Consistency does.
Look for Patterns, Not Perfection
After a week or two of logging, sit down and review your entries. You're looking for repeated themes.
Ask yourself:
- Which meals consistently land you above 180 mg/dL two hours later?
- Which meals keep you steady or bring you back near your starting number?
- Do portion sizes matter more than food type for certain meals?
- Does timing (eating earlier vs. later) change the outcome?
You won't find perfect answers. Blood sugar is influenced by dozens of factors: sleep, activity, stress, hormones, medication timing, and more. But you will start to notice tendencies.
Maybe you'll see that a 45-gram carb breakfast sends you to 210 mg/dL, while a 30-gram version keeps you under 160 mg/dL. That's actionable information you can use. Maybe oatmeal with protein powder behaves differently than oatmeal alone, equally useful.
One common mistake: blaming a single ingredient when portion size is the real issue. Carb counting is harder than it looks, especially when estimating from photos or memory. If a meal spikes you, try logging it again with more precise portions before eliminating it entirely.
Turn Observations Into Small Experiments
Once you spot a pattern, test whether you're right.
Let's say you notice that white rice always pushes your two-hour number above 200 mg/dL. Try swapping in brown rice or cutting the portion in half. Test it the same way: fingerstick before, fingerstick two hours after. Did it make a difference?
Or maybe you notice that eating protein first seems to blunt the spike. Test that theory intentionally. Eat a few bites of chicken before touching the potatoes. See what happens.
This is how meal tracking becomes meal learning. You're not just recording numbers. You're running informal experiments and adjusting based on what you find.
Not every experiment will work. Some meals will surprise you. That's normal. The goal isn't perfect control. It's better awareness.
Use Technology to Make Logging Faster and More Accurate
Manual logging works, but it's tedious. Apps can speed up the process and help you spot trends you might miss in a notebook.
Most diabetes food tracking apps let you search for foods, scan barcodes, and save frequent meals. Some apps, like SNAQ, let you snap a photo of your plate to get instant carb estimates, or speak your meal instead of typing it. These features won't replace careful observation, but they can make consistency easier when life gets busy.
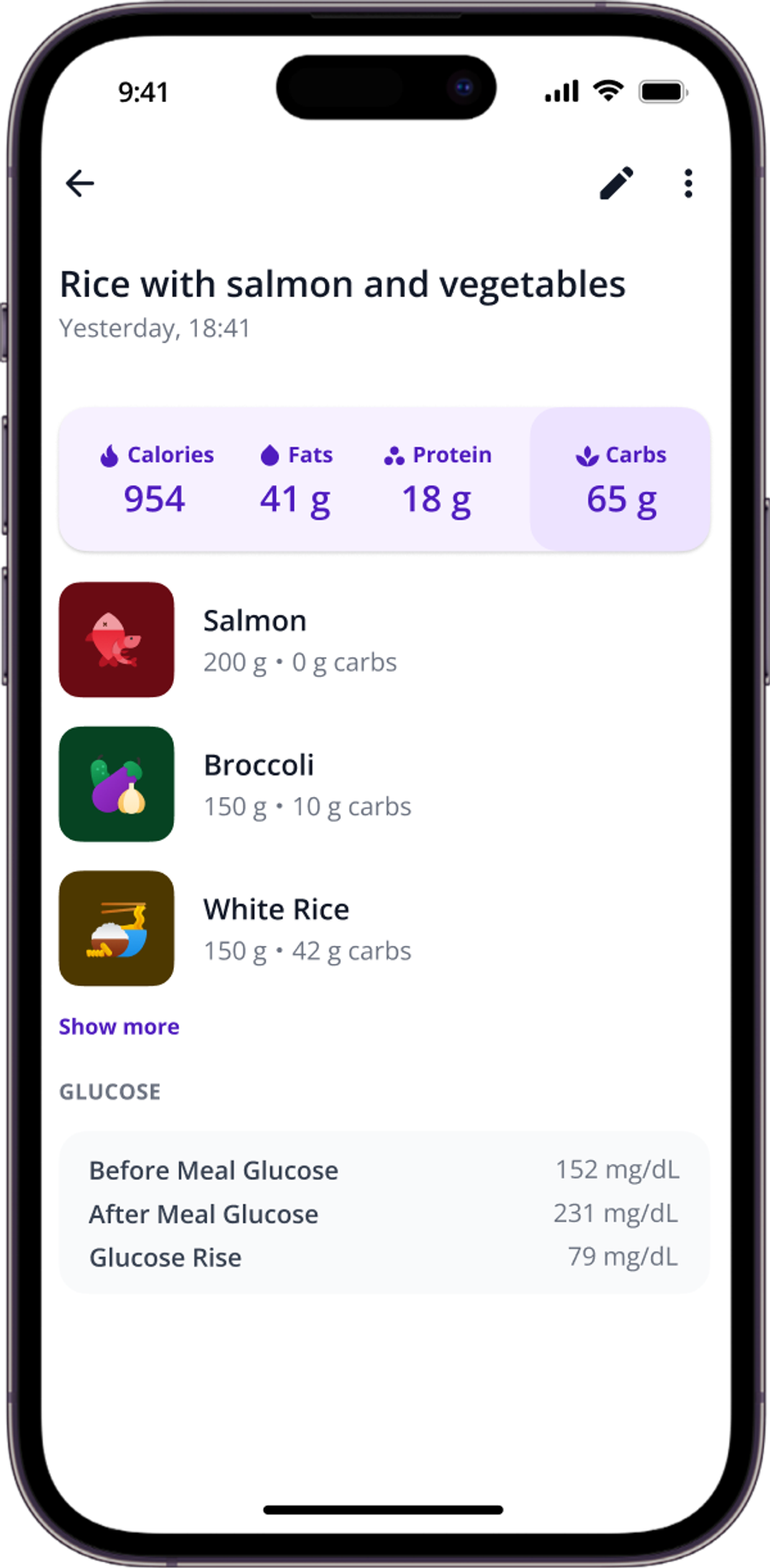
The real value of an app isn't the database. It's the structure it forces. When you log consistently in one place, patterns become visible. You start to notice that your afternoon snack timing matters, or that restaurant portions are larger than you thought.
Accept the Limits of Fingerstick Testing (and Work Around Them)
Fingerstick tests give you snapshots, not the full story. You'll miss the shape of the curve, the timing of the peak, and any dips between tests.
That means you might miss a spike that happened 90 minutes after eating, or a delayed rise that showed up three hours later. You also won't see how quickly your blood sugar came back down.
If a meal feels off but the two-hour test looks fine, try testing again at 90 minutes or three hours. Adjust your timing based on what you learn.
Another limitation: fingerstick accuracy can vary. Factors like unwashed hands, expired strips, or a meter that's out of calibration can skew results. When a number doesn't make sense, wash your hands and retest before changing your approach.
Fingerstick testing isn't inferior. It's different. With structure and repetition, it can teach you a lot.
How SNAQ Fits Into Manual Tracking
If manual logging is slowing you down despite these strategies, here's where SNAQ can help.
AI Photo Analysis lets you snap a picture of your plate and instantly see estimated carb counts and macros. It works best on newer iPhones with LiDAR sensors (Pro models), which improve portion accuracy. You still verify the estimate, but it eliminates most of the guesswork.
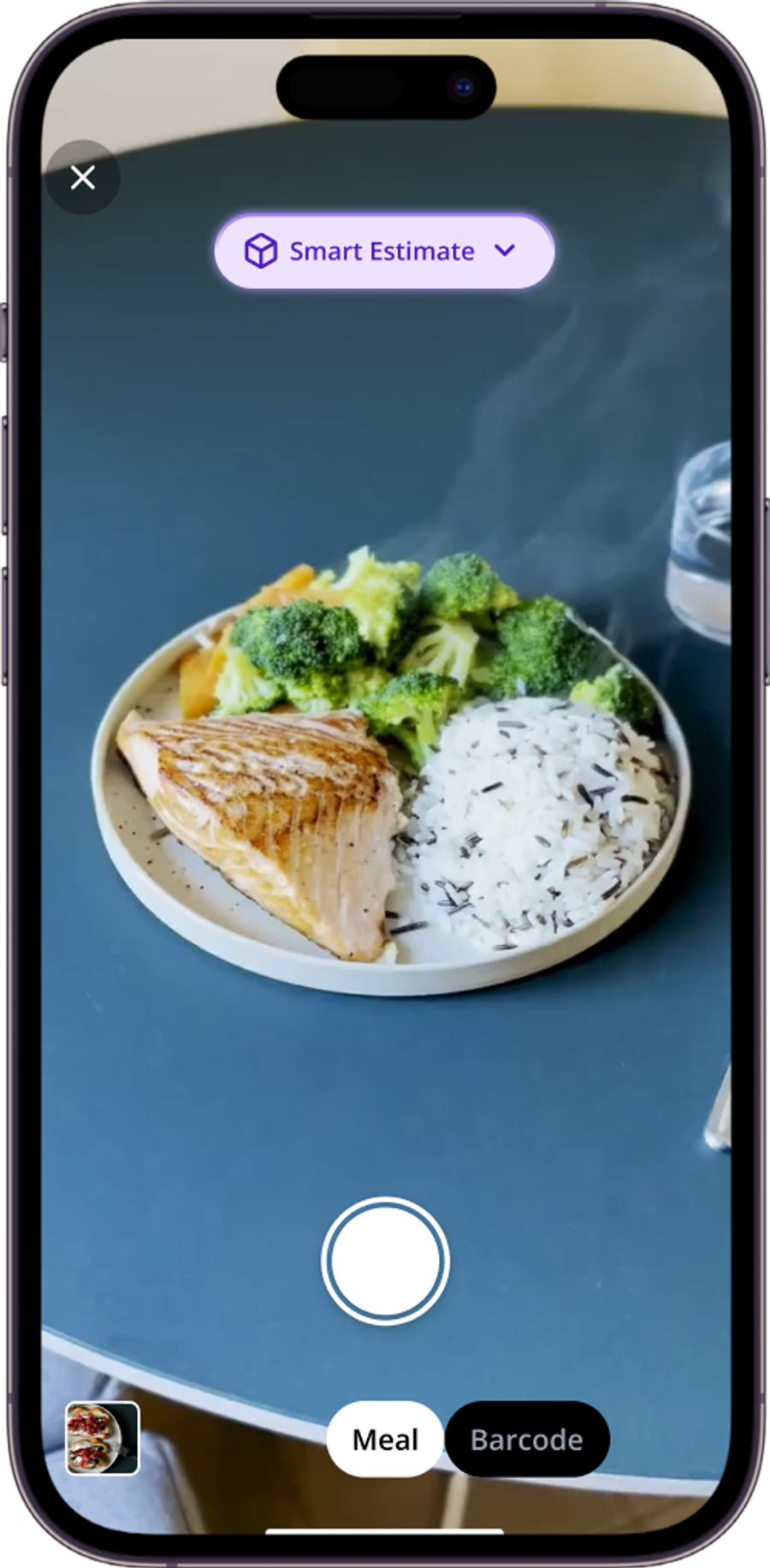
Voice Logging is useful when you're eating on the go. Speak your meal and it logs in seconds. Accuracy depends on how clearly you describe portion sizes, so saying "a cup of rice" works better than "some rice." Barcode Scanning speeds up logging for packaged foods, and Favorites let you save meals you eat often so you don't have to re-enter them every time.
These tools don't replace your testing rhythm or meal analysis. They simply reduce the friction of logging, which makes it easier to stay consistent with the method you've built.
What to Do With What You Learn
Once you've built a clearer picture of how meals affect your blood sugar, you can start making intentional changes.
That might mean adjusting portion sizes, swapping ingredients, changing meal timing, or adding a walk after eating. Small adjustments often add up to noticeable improvements in how you feel and what your meter shows.
Keep testing as you adjust. What worked last month might not work next month. Your body changes. Your routine changes. Meal tracking isn't a one-time project. It's an ongoing feedback loop.
Ready to stop guessing and start learning? Download SNAQ today to turn your smartphone into your smart meal log.
References
The SNAQ website does not contain medical advice. The contents of this website, such as text, graphics, images and other material are intended for informational and educational purposes only and not for the purpose of rendering medical advice. The contents of this website are not intended to substitute for professional medical advice, diagnosis or treatment. Please consult your healthcare professional for personalized medical advice.