Why Some Low-GI Foods Still Spike Your Blood Sugar

You check the glycemic index chart. You choose the low-GI option. You eat a bowl of steel-cut oats or a serving of sweet potato. Then your CGM climbs higher than expected.
It's frustrating. Low-GI foods are supposed to be the safe bet. But the glycemic index is a rough guide, not a personalized prediction. Your body, your portion size, and what else you ate that day all shape how your glucose responds.
This article walks through why some low-GI foods still spike blood sugar and what you can do about it.
The Glycemic Index Doesn't Measure Your Response
The glycemic index ranks foods based on how they raise blood sugar in a controlled lab setting. Participants eat 50 grams of digestible carbohydrate from a single food after fasting overnight. Researchers average the results across the group.
That process creates a useful reference. But it doesn't reflect real meals. You rarely eat one food in isolation. You don't always fast beforehand. And your metabolism isn't identical to the study participants.
Two people can eat the same low-GI food and see completely different glucose curves. Gut bacteria, sleep quality, stress hormones, and recent activity all influence your response. The GI gives you a starting point, but it can't predict what will happen in your body.
A 2015 study from the Weizmann Institute tracked the glucose responses of 800 people eating identical meals. The variation was striking: some participants spiked after eating bread but stayed steady after eating glucose tablets, while others showed the opposite pattern. The researchers found that factors like gut bacteria composition and individual metabolism created responses so different that a food considered "healthy" for one person could spike another's glucose significantly. The study made it clear that population averages can't predict individual response.
Portion Size Changes Everything
A food's GI rating is based on a fixed amount of carbohydrate, usually 50 grams. That might be one cup of lentils or three cups of watermelon. The serving sizes vary wildly.
If you eat twice the reference portion, you're getting twice the carbs. A low-GI food in a large serving can spike your glucose just as much as a moderate-GI food in a smaller portion.
Glycemic load (GL) tries to solve this. It multiplies the GI by the actual grams of carbohydrate in your serving and divides by 100. A low GL is under 10, medium is 11–19, and high is 20 or above.
Focusing on GL instead of GI alone helps you account for realistic portion sizes. But it still doesn't capture individual variability.
Fiber Slows Digestion but Doesn't Stop Spikes
Fiber is one reason many low-GI foods earn their rating. It slows the breakdown of carbohydrates and delays glucose absorption.
But fiber doesn't eliminate glucose. It spreads it out over time. If you eat a large portion of a high-fiber, low-GI food, you may see a delayed rise or a gentler slope, but the total glucose exposure remains.
Some people also experience a secondary spike hours later. This happens when digestion continues and releases glucose that was initially delayed by fiber - a reminder that the body processes food on its own timeline, not always when you expect it.
Food Combinations Shift the Curve
Eating protein, fat, or vinegar alongside carbs can lower the glycemic response. Adding these to a low-GI food may flatten your curve further. But if the low-GI food is already paired with fat (like peanut butter on whole-grain toast), the combination might delay the spike without preventing it.
Some combinations also slow gastric emptying, which extends digestion time. That can help with post-meal fullness but may spread glucose release across several hours.
The same food eaten alone versus in a mixed meal often produces different shapes on your CGM. That variability is normal and one more reason GI tables can't tell the full story.
Stress, Sleep, and Activity All Play a Role
Your glucose response isn't only about the food. Hormones from poor sleep, stress, illness, or your menstrual cycle can raise blood sugar or amplify the effect of carbs.
Here's a concrete example: imagine eating a bowl of oatmeal at 7am after a rough night of sleep. Your stress hormone cortisol is elevated, and your body is less responsive to the carbs. Your CGM might show a steeper spike than usual. Now imagine eating the same bowl on a well-rested morning after a 20-minute walk. Your glucose curve could be noticeably flatter, even though the meal is identical.
Exercise also shifts how your body handles carbs. Recent activity can improve how efficiently your muscles take up glucose, meaning the same low-GI food might produce a smaller spike after a workout than it would on a sedentary day.
These factors shift day to day. That's why a food that worked well yesterday might spike today. Want to dive deeper into these variables? Read our full guide on the factors impacting your glucose levels.
Using CGM to Understand Your Own Response
CGM lets you test foods in real time under real conditions. Instead of relying on population averages, you see how your body responds to specific meals, portions, and combinations.
Over a few weeks, patterns emerge. You might find that quinoa spikes you more than expected, or that lentils work well in smaller portions. You might notice that eating the same oatmeal at breakfast versus dinner produces different curves.
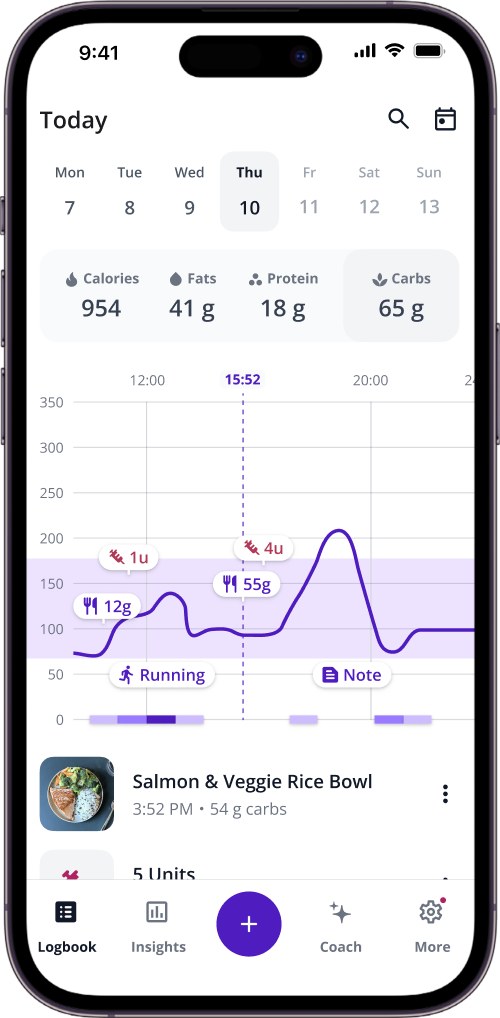
If you're using a tool like SNAQ, your logged meals appear as markers on your glucose graph. You can scroll back through the week and compare how similar foods affected you. The app's Trend Insights feature compiles data across weeks, so you start to see patterns like "lentils work at lunch but spike at dinner" or "sweet potato is fine in half-cup servings." Those insights are specific to you, not a lab average.
New to continuous glucose monitors? Check out our Ultimate CGM Guide 2026: How to Choose the Right Continuous Glucose Monitor to find the best device for your needs.
Practical Strategies for Managing Low-GI Foods
Start with smaller portions of low-GI carbs and check your CGM response. If the spike is mild, you know that portion works. If it's higher than expected, try cutting the serving size or pairing the food with protein or fat.
Pay attention to timing. Some people tolerate carbs better earlier in the day, while others do better in the evening. Your pattern may differ.
Keep a short list of low-GI foods that work well for you. Not every low-GI option will fit your metabolism. Personalize your go-to staples based on CGM feedback, not just GI rankings.
If you're experimenting with new foods, test them one at a time. That way you can isolate the effect without confounding variables.
For faster logging, SNAQ's AI Photo Analysis can estimate carb and macro content from a photo; on iPhones with LiDAR (Pro models), depth sensing improves portion accuracy. It's not perfect, but it gives you a reference point to compare against your CGM response without manual carb counting. Voice logging is also available if you want to describe your meal out loud and edit later.

Takeaway
Low-GI foods are a useful starting point, not a guarantee. Your glucose response depends on portion size, food pairings, and daily factors that GI tables can't capture.
Track a few low-GI staples with your CGM to see which ones actually keep you stable. Compare glycemic load, not just GI, when planning portions. Test the same food at different times of day and in different combinations to find your patterns.
If you want help spotting those patterns, SNAQ overlays your meals on your glucose graph and highlights trends across weeks. It's built to help you see which foods actually work for your body, not just which ones rank well on a chart.
Ready to close the gap between your carb counts and your CGM? Download SNAQ on App Store or Google Play and start logging your next meal.
Frequently Asked Questions
References
- Atkinson FS, Foster-Powell K, Brand-Miller JC. International Tables of Glycemic Index and Glycemic Load Values 2023. Diabetes Care, 2023.
- Jenkins DJ, Wolever TM, Taylor RH, et al. Glycemic index of foods: a physiological basis for carbohydrate exchange. Am J Clin Nutr, 1981
- Liu S, Willett WC, Stampfer MJ, et al. A prospective study of dietary glycemic load, carbohydrate intake, and risk of coronary heart disease in US women. Am J Clin Nutr, 2000.
- Beck RW, Riddlesworth TD, Ruedy KJ, et al. Continuous Glucose Monitoring Versus Usual Care in Patients With Type 2 Diabetes Receiving Multiple Daily Insulin Injections. Diabetes Care, 2017.
- Polonsky WH, Hessler D, Ruedy K, Beck RW. The Impact of Continuous Glucose Monitoring on markers of quality of life. Diabetes Care, 2017.
- Zeevi D, Korem T, Zmora N, et al. Personalized Nutrition by Prediction of Glycemic Responses. Cell, 2015.
The SNAQ website does not contain medical advice. The contents of this website, such as text, graphics, images and other material are intended for informational and educational purposes only and not for the purpose of rendering medical advice. The contents of this website are not intended to substitute for professional medical advice, diagnosis or treatment. Please consult your healthcare professional for personalized medical advice.
Questions, inputs or feedback? We are happy to hear from you at feedback@snaq.io or check out our website at snaq.io to find out more!




